The Placebo Effect
The placebo effect officially entered the medical world in the late 1700s: Dr. William Cullen was one of the first physicians to use the term placebo. In a 1772 lecture, he described prescribing a placebo to a patient he thought to be incurable. Specifically, he prescribed an active placebo (which would mimic the side effects of a drug without treating the condition), as opposed to an inactive substance such as a sugar pill. In the mid 1900s, placebos became a commonplace control in the medical world because randomized controlled trials became the gold standard for medical testing. After the Second World War, a greater emphasis on informed consent discouraged use of placebos as a treatment.
How Do Placebos Work?
The placebo response is a result of a patient’s expectations and social cognition. Despite having no effect to treat the patient’s illness, placebos are administered in a medical context. Patients have an expectation that they will get help because of this context. This elicits a response from the brain that decreases pain and stress (Fun fact: a placebo that elicits a negative response is called a nocebo). Placebo analgesia (reduced pain) is associated with the autonomic nervous system and the endocrine system, indicating that the placebo effect has physiological pathways. A 2013 study by Stephan Geuter and Christian Büchel found that nocebo treatments can activate pain-facilitating mechanisms in the spinal cord. Verbal nocebo treatments have been associated with hyperactivity in the neuro-endocrine system and increased levels of cortisol and adrenocorticotropic hormone. This all points to the fact that the placebo response is not purely psychological and is also rooted in neurobiology.
Placebos as a Potential Treatment
While placebos do not work to cure an underlying condition, they do help with somatic symptoms such as pain and nausea. In fact, placebo treatments have been recorded to improve motor skills in Parkinson’s disease patients due to increased dopamine release. Additionally, the difference between placebos and antidepressants is modest when looking at mild to moderate depression. This is important because it means that placebos could potentially serve as a supplement to drugs.
Does knowledge of a placebo impact its effect?
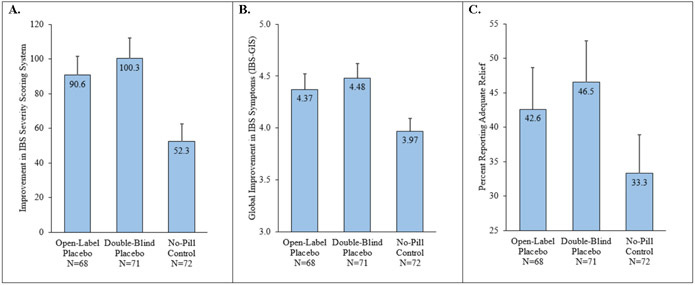
One barrier to the use of placebos as a treatment is patient-provider transparency. Since placebos seemingly work due to the expectation that the treatment will improve symptoms, it stands to reason that knowingly taking a placebo would eliminate its effectiveness. This poses ethical concerns as if a physician tells a patient that a placebo is an active drug when it actually isn’t, there is a breach of trust. Interestingly however, the placebo response holds even when a patient is aware that they are taking a placebo. A 2021 study by Lembo et al. compared the progression of Irritable Bowel Symptoms across three groups: no pill, open label placebo, and a double-blind placebo.
What they found was that the group that knew they were taking a placebo still showed improvement in symptoms compared to the group that took no pill, as seen in the above figure. Open label placebos have also been shown to improve outcomes in opioid use disorder and chronic lower back pain. While open label placebos may not be as effective as double-blind placebos, the lack of deception makes them a promising method to alleviate patient symptoms.
Ultimately, placebos are a testament to the versatility of the human brain. It is important to continue researching both placebo and nocebo responses because understanding how our brains respond to placebos can help improve understanding of disease pathways and how to treat them.